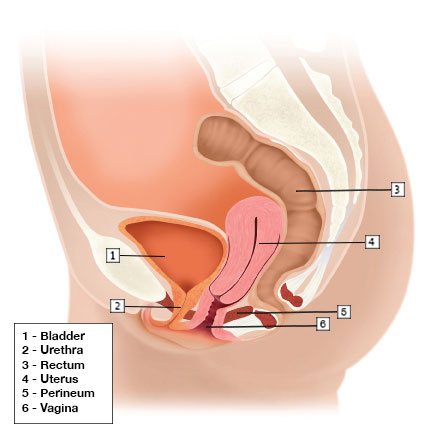
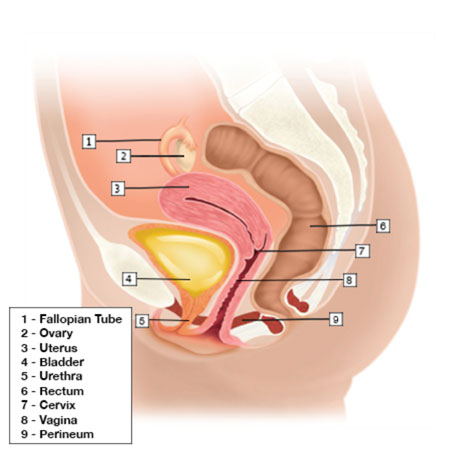
Uterine Prolapse/Pelvic Organ Prolapse occurs when pelvic floor muscles and ligaments stretch and weaken. This weakening of the support structures allows the uterus to move out of its normal position and drop into the vagina. Uterine prolapse may shorten the length of the vagina, or even fall down far enough to protrude through the vaginal opening.
Uterine Prolapse
Symptoms can include:
- Sensation of heaviness or pulling in your pelvis
- A bulge protruding from your vagina
- Pain with sexual activity
- Difficulty inserting tampons
- Low back pain
The three main factors that contribute to the development of Uterine Prolapse are:
- Hereditary factors. Uterine Prolapse can run in families. There are genes that code for the supporting structures of the uterus and variations in these genes can lead to a weakening of the pelvic floor.
- Childbirth. Vaginal birth can stretch and weaken the supporting structures of the uterus.
- Age. As supporting structures of the uterus age, they weaken.
Book An Appointment
I was treated by Dr. George Shashoua for Cystocele, Rectocele, Uterine Prolapse and Urinary Incontinence. The procedures were explained to me on my first visit, and I was told what to expect after surgery. All went as expected.
Dr. Shashoua and his staff (I worked mostly with Marissa and Kristin) are very caring and supportive. I never called with a question that I wasn't given an answer or given a return call soon by one of the staff. The atmosphere in the office is always very calm and friendly. Miranda at the front desk always greets you with a smile and by name. I highly recommend Dr. Shashoua.
-Mary G.
Diagnosis of Uterine Prolapse
Uterine Prolapse is diagnosed by pelvic exam. Often times, when there is uterine prolapse, other defects of the pelvic floor are also present, such as cystocele or rectocele.
Treatment of Uterine Prolapse
Treatment of uterine prolapse ranges from no treatment for a small, asymptomatic prolapse to a pessary or surgical repair for a more advanced prolapse.
There are a number of ways to treat symptomatic uterine prolapse. Some women choose to treat uterine prolapse with a pessary. A pessary is a vaginal support device used to elevate the prolapse by occupying space in the vagina. A pessary is typically used in women who are not candidates for surgery due to age or poor health.
Surgery is elective and is done to relieve symptoms and restore the anatomy of the vagina. Symptoms of prolapse do not decrease without treatment. Surgery to treat uterine prolapse may include supracervical or complete hysterectomy, often in combination with da Vinci sacrocolpopexy or uterosacral colpopexy.
Got questions? Need an appointment? We’re here to help!